Focused Assessment: Scroll down all theassessments (pages 1-5) and see if the assessment data is truly "focused". IOW: Everything that relates to the problem statement is listed, but no extraneous information is included

Vital signs and significant history: The vital signs tell us that Mr. Culver may have an acute problem (T 100.2, 102 and irregular and respiratory rate of 30 indicate he is "toxic", i.e., sick! But the most alarming data in the vital signs, is the refractory hypoxemia (%sat = 85 on 4 liters of oxygen by nasal prongs. (To understand the significance of this, click on the button to go to the page where this is explained.) The significant history is put here (in Focused Assessment) instead of Brief Description... because it is directly relevant to the problem statement. It is assessment... not just background. That history includes the fact that he has an extensive smoking history, states he "quit" 2 weeks ago (really?) Mr.Culver had an episode of respiratory failure last year and only just now quit smoking? So these initial findings suggest our patient has an "acute on chronic" condition. He has permanently damaged lungs (Chronic obstructive pulmonary disease) and may have an acute pulmonary infection.
The nurse has included assessments of Mr. Culver's heart function. Is this relevant to the problem statement?
Yes! The long-term damage to Mr. C's lungs have had profound consequences for his heart. In fact, he has a particular kind of right sided heart failure seen in patients with chronic hypoxia called Cor Pulmonale. Therefore, the nurse has listed observations commonly seen in this type of heart failure. Because the right side of Mr. C's heart is struggling to push blood into his diseased lungs, the right ventricle and right atrium are over-filled with blood. Therefore venous drainage from the head and brain is impeded. This produces bulging of the jugular veins. Because the right atrium is stretched, conduction pathways from the SA node are distorted. For this reason the most common arrhythmia seen in patients with Cor Pulmonale is premature atrial contractions (PAC's). Furthermore, because the right side of the heart is overfilled with blood, venous return from the rest of his body (legs, gut, liver, scrotum, etc.) is impeded. This produces increased hydrostatic pressure in these tissue beds which in turn, causes fluid to seep out of the veins and capillaries and into the interstitial spaces. This produces peripheral edema, easily observed in his lower legs and feet. Not uncommonly, nutrition is adversely influenced by right sided heart failure because the gut has become edematous and hypoactive. Similarly, these patients have portal hypertension. The liver is edematous and venous drainage from the gut cannot easily flow into and through the liver. As a result, Mr. C is not hungry, can't really eat, and even if he did, his liver would not be able to metabolize the nutrients he consumed. Why then, you might ask... has he been able to gain 2 pounds since he was admitted to the hospital? The answer is, of course, that he is retaining water. He is edematous.
Other observations: Mr. C. cannot lay down. He's OK when he's sitting at about a 45 degree angle, but if he is more supine, he gets very uncomfortable. Recall from our discussion of COPD pathophysiology that Mr. C's lungs are overinflated. For years he's destroyed (by smoking) the pulmonary architecture that keeps small airways open. For this reason, he has been progressively unable to exhale all the breath he inhales. We can see this with our eyes when we see his barrel chest. We also observe on a simple x-ray that Mr. C's diaphagms are flat. In this mechanically unfavorable condition, the diaphragms aren't able to contribute to air movement into and out of Mr. C's lungs. So Mr. C. must assume the position that is most comfortable for him. Lying flat on his back is out of the question because this causes abdominal contents to press up against the flattened diaphragm making inspiration even more difficult. The nurse notes that he can tolerate a chair but assumes a tripod position when he does. The reason for this is that he must use accessory muscles of respiration (sternoclaidomastoid, trapezius) to inhale. This is fatiguing. By leaning forward and propping his elbows on some surface he puts these muscles in a more energy efficient position. The nurse also notices one of the absolutely classical signs of airway obstruction and that is use of abdominal muscles during the expiratory phase. In health, expiring/exhaling air is completely passive. It is not so for Mr. C. and never will be again... he has to work very hard for each breath. (Read more by clicking the button below.)
Other observations: Mr. C. cannot lay down. He's OK when he's sitting at about a 45 degree angle, but if he is more supine, he gets very uncomfortable. Recall from our discussion of COPD pathophysiology that Mr. C's lungs are overinflated. For years he's destroyed (by smoking) the pulmonary architecture that keeps small airways open. For this reason, he has been progressively unable to exhale all the breath he inhales. We can see this with our eyes when we see his barrel chest. We also observe on a simple x-ray that Mr. C's diaphagms are flat. In this mechanically unfavorable condition, the diaphragms aren't able to contribute to air movement into and out of Mr. C's lungs. So Mr. C. must assume the position that is most comfortable for him. Lying flat on his back is out of the question because this causes abdominal contents to press up against the flattened diaphragm making inspiration even more difficult. The nurse notes that he can tolerate a chair but assumes a tripod position when he does. The reason for this is that he must use accessory muscles of respiration (sternoclaidomastoid, trapezius) to inhale. This is fatiguing. By leaning forward and propping his elbows on some surface he puts these muscles in a more energy efficient position. The nurse also notices one of the absolutely classical signs of airway obstruction and that is use of abdominal muscles during the expiratory phase. In health, expiring/exhaling air is completely passive. It is not so for Mr. C. and never will be again... he has to work very hard for each breath. (Read more by clicking the button below.)
Finally, the nurse observes that Mr. C. is coughing up yellow sputum. This is not normal for the patient. He does have a chronic cough, he does produce sputum. But something caused Mr. C. to have an acute exacerbation of respiratory failure. The yellow sputum is a tip-off that he has gotten infected. The nurse adds this observation to the Mr. C's vital signs and an infective source of the failure looks even more likely. (The nurse will cinch the deal by looking at the patient's white count and differential. But we'll get to that is a bit.)
The nurse now gets out a stethoscope to do a more thorough physical assessment.
The nurse now gets out a stethoscope to do a more thorough physical assessment.
How to listen to breath sounds:
When you listen to a chest you should do it systematically:
First: Don't listen... look! What is the ratio represented by the length of time it takes the patient to breathe in vrs. the time it takes to breathe out. Even in healthy lungs, inspiration is shorter than exhalation. It takes roughly 1/3 longer to exhale than inhale. Mr. C. spends a very long period of time trying to breathe out and then snatches a brief inhalation.
Second: note the underlying type of breath sound. There are three types. Vesicular breath sounds are what you should hear when listening over normal, healthy lung tissue. You will typically hear the whole inspiratory phase, but only the first 1/3 of the expiratory phase. Stated another way, the inspiratory phase should sound like it's 3 times longer than the expiration. (It's not... but it sounds that way.) The worst (most unhealthy) type of underlying breath sound is called bronchial breath sounds. Sounds are conducted through solids more easily than air. When listening over a lung field that is filled with fluid and infective goop, the breath sound is harsh and you're able to hear the entire expiration. In fact, sometimes it's called a "tubular" breath sound because is sounds like someone blowing through a tube. (If you want to hear "bronchial" breath sounds put your stethoscope over your trachea and breathe in and out. You'll hear the entire breath, and a distinct pause between inspiration and expiration.) The third type of breath sound is bronchovesicular. If you listen to an area of lung that is a mixture of some aerated alveoli and some that are fluid-filled, you get a hybrid sound. Like bronchial, the sound of inspiration and expiration are equal in length of time. However, the two phases just roll into each other. There is not a distinct "pause" between inspiration and expiration.
Third: Take note of extra sounds (sometimes called "adventitious" sounds). Rhonchi: Low pitched wheezes that are heard during both phases of the respiratory cycle. Course crackles are discrete popping sounds that are fairly loud and low pitched. Early inspiratory crackles (rales) are just like their name implies. They are heard during the early phase of inspiration. Sometimes they are cleared by cough. Late inspiratory crackles begin in the last moments of the inspiratory phase. They kinda sound like velcro being pulled apart. Wheezes have a "musical" quality, and may sound high pitched (like a squeak) or low (like a moan.) They indicate tight, constricted airways and the degree of constriction correlates roughly to the % of the time during the respiratory cycle the wheezes are heard. There are other types of wheezes (monophonic and polyphonic) that when heard suggest the type and seriousness of airway constriction.
Please take 6-7 minutes and listen to these breath sounds in an excellent tutorial from Youtube.
First: Don't listen... look! What is the ratio represented by the length of time it takes the patient to breathe in vrs. the time it takes to breathe out. Even in healthy lungs, inspiration is shorter than exhalation. It takes roughly 1/3 longer to exhale than inhale. Mr. C. spends a very long period of time trying to breathe out and then snatches a brief inhalation.
Second: note the underlying type of breath sound. There are three types. Vesicular breath sounds are what you should hear when listening over normal, healthy lung tissue. You will typically hear the whole inspiratory phase, but only the first 1/3 of the expiratory phase. Stated another way, the inspiratory phase should sound like it's 3 times longer than the expiration. (It's not... but it sounds that way.) The worst (most unhealthy) type of underlying breath sound is called bronchial breath sounds. Sounds are conducted through solids more easily than air. When listening over a lung field that is filled with fluid and infective goop, the breath sound is harsh and you're able to hear the entire expiration. In fact, sometimes it's called a "tubular" breath sound because is sounds like someone blowing through a tube. (If you want to hear "bronchial" breath sounds put your stethoscope over your trachea and breathe in and out. You'll hear the entire breath, and a distinct pause between inspiration and expiration.) The third type of breath sound is bronchovesicular. If you listen to an area of lung that is a mixture of some aerated alveoli and some that are fluid-filled, you get a hybrid sound. Like bronchial, the sound of inspiration and expiration are equal in length of time. However, the two phases just roll into each other. There is not a distinct "pause" between inspiration and expiration.
Third: Take note of extra sounds (sometimes called "adventitious" sounds). Rhonchi: Low pitched wheezes that are heard during both phases of the respiratory cycle. Course crackles are discrete popping sounds that are fairly loud and low pitched. Early inspiratory crackles (rales) are just like their name implies. They are heard during the early phase of inspiration. Sometimes they are cleared by cough. Late inspiratory crackles begin in the last moments of the inspiratory phase. They kinda sound like velcro being pulled apart. Wheezes have a "musical" quality, and may sound high pitched (like a squeak) or low (like a moan.) They indicate tight, constricted airways and the degree of constriction correlates roughly to the % of the time during the respiratory cycle the wheezes are heard. There are other types of wheezes (monophonic and polyphonic) that when heard suggest the type and seriousness of airway constriction.
Please take 6-7 minutes and listen to these breath sounds in an excellent tutorial from Youtube.
In addition to listening to Mr. C's lungs, the nurse tries to hear his heart sounds. As noted in the assessment data, the nurse thinks there might be an S3. This would not be surprising since Cor pulmonale (Rt. sided heart failure) is often associated with severe and/or advanced COPD. Note that the S3 of right heart failure is best heard on the left lateral sternal border. Also, a tip: Use the bell of your stethoscope with very light pressure.
Which lab values are important to assess?
The first labs the nurse considers are the chemistries found on the BMP (basic metabolic panel) and CMP (complete metabolic panel). First the nurse notices that Mr. C may be dehydrated because his creatinine and BUN and also his serum sodium are all high, or on the high side of "normal". The patient's liver studies (ALT/AST) are somewhat elevated. This is not surprising to the nurse because right sided heart failure will cause fluid back up into all the viscera, including the liver. The patient's albumin is low, again, not surprisingly since albumin is sythesized in the liver. But why is the calcium low? Albumin and calcium levels usually pair each other since most of the calcium we measure is attached to albumin molecules. BUT... the most revealing serum chemistry the nurse notes is the bicarbonate (HCO3). This value is very much higher than it should be. The reason for this is that Mr. C. lives moment to moment with an elevated PaCO2, that is, he is almost always in respiratory acidosis from one degree to another. In order to compensate for this acidosis the kidneys are retaining bicarbonate ions and not letting them leave in the urine. Therefore, the presence of an elevated HCO3 not only tells the nurse that the patient is retaining (failing to exhale and get rid of) CO2. Not only that, but it means this has been going on for some time. It is a long-term adaptation to respiratory acidosis.
Next the nurse looks at the hematology studies and picks up some serious information. First, Mr. C's hgb and hct are on the high side. Is that good or bad? They are elevated because Mr. C is a little dehydrated. If he had a normal fluid volume, these constituents of blood would be a bit more diluted and would measure a little lower. BUT... there is another reason a patient with chronic lung disease would have a high hct/hgb. Mr. C. is chronically hypoxic. Under these conditions his kidney's mistakenly assume that he is anemic. They release erythropoitin, which makes Mr. C's bone marrow generate more RBC's. This causes a relative "polycythemia". Next the nurse looks at the WBC and here finds some very useful numbers. The white count is up and the % of neutrophils in the WBC is higher than normal. These findings are called neutrophilia" and suggests a "left shift" which is almost always associated with a bacterial infection. To learn much more about this, go to the discussion of inflammation
Next the nurse looks at the hematology studies and picks up some serious information. First, Mr. C's hgb and hct are on the high side. Is that good or bad? They are elevated because Mr. C is a little dehydrated. If he had a normal fluid volume, these constituents of blood would be a bit more diluted and would measure a little lower. BUT... there is another reason a patient with chronic lung disease would have a high hct/hgb. Mr. C. is chronically hypoxic. Under these conditions his kidney's mistakenly assume that he is anemic. They release erythropoitin, which makes Mr. C's bone marrow generate more RBC's. This causes a relative "polycythemia". Next the nurse looks at the WBC and here finds some very useful numbers. The white count is up and the % of neutrophils in the WBC is higher than normal. These findings are called neutrophilia" and suggests a "left shift" which is almost always associated with a bacterial infection. To learn much more about this, go to the discussion of inflammation
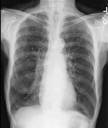
The nurse is informed by how the radiologist reads Mr. C's chest film. Since the information there confirms many of his/her observations, it is included in the assessment data. The same is true for the information provided by the cardiologists reading of the 12-lead.
After the nurse has studied diagnostics, lab studies, gotten physical findings and made important observations, it's time to give the patient a little time to talk. The nurse doesn't ask a lot of "yes"/"no" questions, but rather uses open ended questioning techniques. Principally the nurse asks Mr. C. questions to elicit information about his quality of life and what symptoms made him decide to come to the hospital. As you can see from the quotes in the assessment column, the patient was more than willing to share this information with the nurse.
From all this rich and abundant assessment data the nurse develops three potential nursing diagnoses. Click on the button below and see if you believe they are appropriate for the data that was collected.
After the nurse has studied diagnostics, lab studies, gotten physical findings and made important observations, it's time to give the patient a little time to talk. The nurse doesn't ask a lot of "yes"/"no" questions, but rather uses open ended questioning techniques. Principally the nurse asks Mr. C. questions to elicit information about his quality of life and what symptoms made him decide to come to the hospital. As you can see from the quotes in the assessment column, the patient was more than willing to share this information with the nurse.
From all this rich and abundant assessment data the nurse develops three potential nursing diagnoses. Click on the button below and see if you believe they are appropriate for the data that was collected.
